If you have a Non-Healing Diabetic Foot Ulcer you need to seek treatment immediately! Don’t wait any longer. Reassured by Plastic Surgeron expert Dr. Kai Kaye from Ocean Clinic Marbella. It’s important to take a diabetic foot ulcer seriously.
There are effective treatments for foot ulcers that are designed to avoid amputation due to diabetes. If you seek treatment early, you will increase the likelihood that your ulcer may heal.
If you’ve been diagnosed with diabetes, you probably already know you need to take care of your feet. Your doctor has likely told you to pay particular attention to any non-healing foot cuts or sores you notice. And then it happens: one day you may be looking down and find yourself wondering “how long has that sore been there?”
This article aims to give you answers and solutions about how to treat it and what you have to do next…
Diabetic Foot Problems: Symptoms, Treatment, and Care
Do you think you may have/suffer from a diabetic foot ulcer – What should I do? What is a diabetic foot ulcer? Should I be concerned? These and more questions arise when you confront a diabetic foot ulcer. If you’ve thought about any of these questions. It may be the time the right time to consider talking to your doctor. First, we suggest you book an appointment with your diabetic doctor and then you can make an appointment either with
Dr. Kaye from Ocean Clinic Marbella or Dr. Fakin Madrid or Zürich Ocean Clinic, Here:
Diabetic foot ulcers are sores on the feet or anywhere below the ankle that someone with diabetes may develop. If you have diabetes and you have an open sore on your foot that just won’t heal, it’s red, painful, and warm. It’s draining pus, smells funny, or just doesn’t seem to get better then you may have a non-healing diabetic foot ulcer.
What is a diabetic foot ulcer?
Diabetic foot ulcers are wounds present on the foot or below the ankle, which do not heal. [i] The presence of these ulcers is a leading cause of amputation due to diabetes. Just in the USA, The Centers for Disease Control and Prevention estimates that about 73,000 lower-limb amputations, not related to trauma, are performed every year on people with diabetes.
This is why if you’re living with diabetes and have a sore, or an open area, on your foot that presents the following symptoms:
• doesn’t appear to be healing
• is red
• is hot to the touch
• is draining pus
• or just keeps coming back
You may have a non-healing diabetic foot ulcer and should make an appointment with your doctor as soon as possible.
We’ve found that on average people tend to wait, as well as how long they typically wait, before going to the doctor. One scientific study found that ulcers that have been present for about a month and a half before the first doctor visit were less likely to heal than ulcers that were seen and treated sooner.
Non-Healing Foot Ulcers and Peripheral Artery Disease (PAD)
• Foot Ulcers may be a sign that you may have peripheral artery disease (PAD). PAD develops when the build-up of plaque in the arteries of the limbs, typically the legs, decreases the amount of blood and oxygen getting to your legs and feet.
How does Foot Ulcer develop?
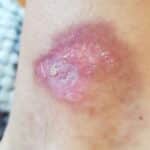
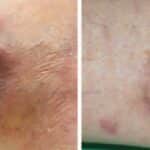
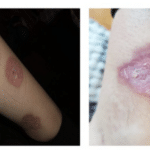
Stage I Ulcers usually begin as an area of redness on the skin. The area may have a different firmness or temperature than the surrounding skin or may be painful to the touch, similar to a blister.
Stage II Over time, the skin will break down, exposing a shallow wound bed, followed by a
Stage III A layer of fat beneath the skin, until bones, tendons, or muscles are exposed
Stage IV Alternatively, the ulcer may be covered with discolored tissue (ranging from yellow to green to brown or black), making it impossible to determine the extent of the damage simply by looking at the ulcer.
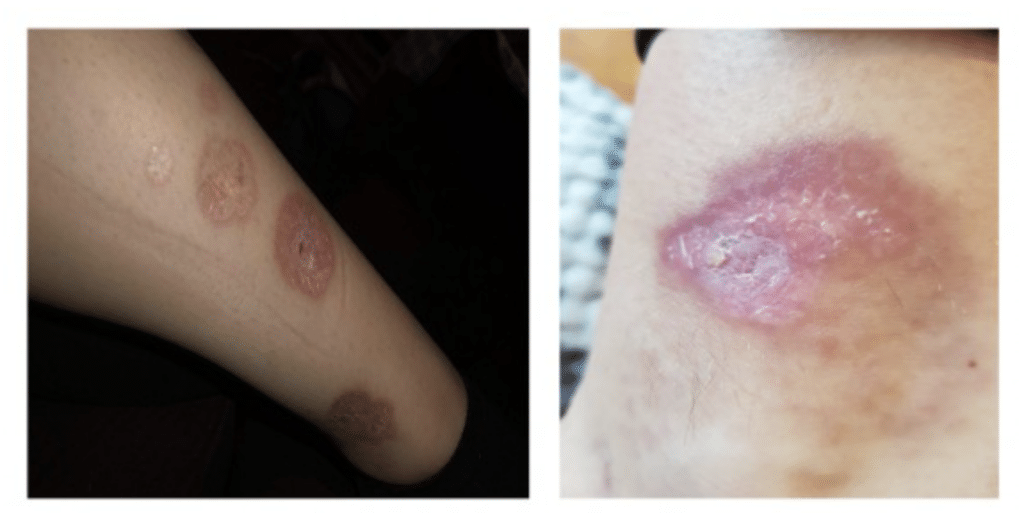
How does Diabetic Leg Ulcer develop? Photo of a 1st and 2nd stage. April 2020
The following conditions make the development of an ulcer more likely:
Diabetic neuropathy is one of the most common complications of diabetes, as well as one of the leading causes of diabetic foot ulcers.
• Diabetic neuropathy results from damage to the nerves in the arms and legs. You may notice either tingling or the loss of feeling in your feet. Neuropathy usually:
• Begins in the toes
• Occurs on both sides
• Progresses up the legs
• Neuropathy can also change how you use your feet to walk and, over time, this can lead to changes in the actual shape of your feet. These changes increase your risk of ulceration as well.
What Causes Diabetic Foot Ulcer?
Often an ulcer forming in a patient with diabetes: Diabetic neuropathy – Diabetes can cause damage to nerves in parts of the body, particularly the feet. It’s one of the most common complications experienced by people living with diabetes. This damage to the nerves can alter sensation in the feet, resulting in anything from increased sensitivity and pain to tingling and complete loss of sensation.
How Do You Treat Diabetic Leg-Ulcers?
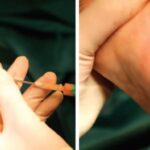
Unless treated promptly, diabetic foot ulcers may cause complications that include cellulitis, osteomyelitis (bone infections), and gangrene. Advanced foot ulcers often require wound debridement, a process that carefully removes dead tissue. Doctors perform debridement in various ways one of which is probing the wound to determine the size of the ulcer.
Tight control of blood glucose levels is critical during the effective treatment of a diabetic foot ulcer.
Diabetic Leg Ulcer Surgery Fat Transfer Stem Cell reconstructive surgery:
Ocean Clinic Plastic surgeon Dr. Kai Kaye has treatment for diabetic leg ulcers!
Diabetes mellitus or Diabetic Leg Ulcers can be a very complicated condition to keep under control, and long-term patients can develop further complications. One of those risks is a diabetic foot, which often occurs because of diabetes that was not taken care of properly. It forms because the tissue is breaking down. After all, the blood circulation is irregular because of the disease, leaving the area unprotected, which can lead to ulcers appearing. In case ulcers are neglected, they can become infected, which can present a danger to health, ending up in amputation in the most severe cases.
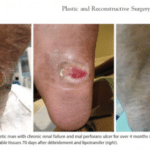
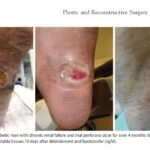
We have learned from Ocean Clinic the result of a study #Debridement and Autologous Lipotransfer (fat grafting, lipofilling) for Chronic Ulceration of the Diabetic Foot and Lower Limb Improves Wound Healing# published in the journal of the American Society of Plastic Surgeons. The study was using 30 patients(17 men and nine women) with a median age of 59 years (range, 25 to 85 years) and an average body mass index of 26.9 ± 10.4 kg/m2. Sixteen of these were diabetics (type 1 or type 2).
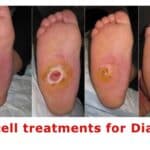
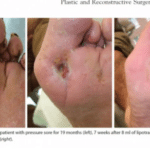
During the results of the study the fat grafting treatment, twenty-two of 25 wounds (88 percent) healed completely within a mean of 68.0 ± 33.0 days. A reduction of wound size by 50% was achieved after an average of 4 weeks. In one patient with an ulcer within particularly scarred tissues on the lower limb, a repeated session of lipotransfer led to complete wound healing after another 4 weeks.
The methods used during this study consisted of twenty-six patients with nonhealing wounds who were treated with surgical débridement and autologous lipotransfer (using the débridement and autologous lipotransfer method). The mean age of the wounds before the intervention was 16.7 months. Wound size after débridement averaged 5.1 ± 2.6 cm2. On average, 7.1 ± 3.3 ccs of lipoaspirate was transferred into the wound area.
The primary aim of their study was to assess the time until complete wound closure was achieved. The secondary aim was to measure the time taken for a reduction in wound size by 50 percent.
What to do if You Have Non-Healing Diabetic Foot Ulcer?
If you’re concerned that you have a non-healing diabetic foot ulcer, make an appointment to see your doctor, and read more to educate yourself about this subject. From this article, we hoped you’ve learned some basics and acquired more information.
First, we suggest you book an appointment with your diabetic doctor and then make an appointment with
Dr. Kaye from Ocean Clinic Marbella or Dr. Fakin Madrid or Zürich Ocean Clinic
now you can book an appointment online here
through the website www.oceanclinic.net, you will get information and answers to your questions easily and comfortably without travelling abroad. Ocean Clinic Online consulting is a simple and fast way to get answers to your concerns.
DIABETES general worldwide information:
Diabetes is a 21-century epidemic, and it is rising, we have already 422 million adults have diabetes. This is 1 person in 11. 3.7 million deaths due to diabetes and high blood glucose. 1.5 Million from these deaths caused by diabetes
Complication Of Diabetes:
• High blood sugar fluctuations can lead to serious complications.
• Over time, diabetes can damage the heart, blood vessels, eyes (blindness), kidneys, and nerves.
• Amputation of a lower limb is the most common complication of diabetes
• Every year in UK 7500 diabetics have leg amputation and in Mexico 75000 persons per year.
• According to the American Diabetes Association, worldwide, a person loses a limb due to diabetes-related complications every 30 seconds.
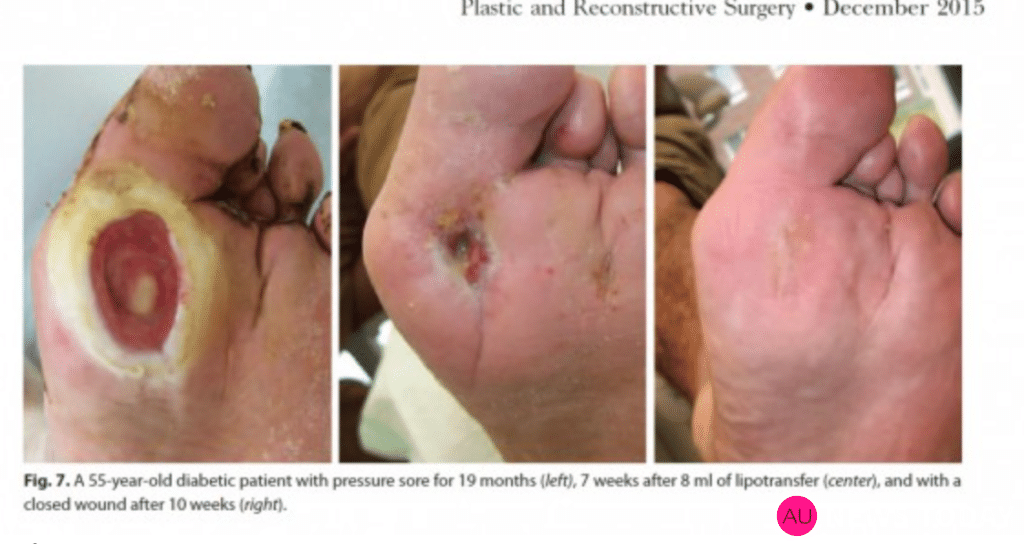
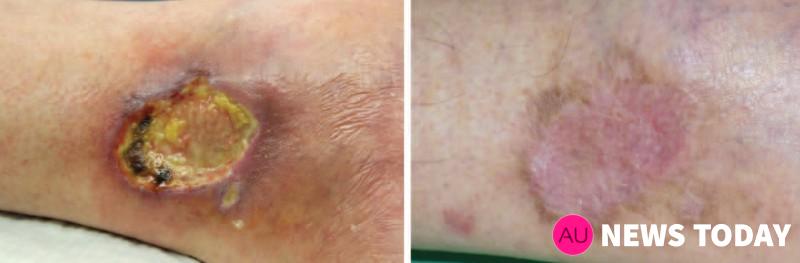
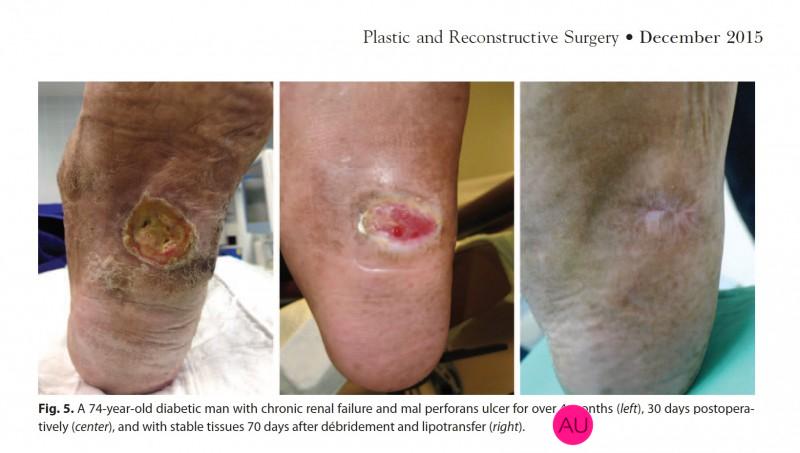
Débridement and Autologous Lipotransfer (fat grafting, lipofilling) for Chronic Ulceration of the Diabetic Foot and Lower Limb Improves Wound Healing reconstructive surgery
Sources
[i] American Diabetes Association. Consensus Development Conference on Diabetic Foot Wound Care: 7-8 April 1999, Boston, Massachusetts. American Diabetes Association. Diabetes Care. 1999;22:1354-1360.
[ii] Centers for Disease Control and Prevention. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014, Atlanta, GA: US Department of Health and Human Services; 2014. http://www.cdc.gov/diabetes/data/statistics/2014statisticsreport.html (accessed 8/1/2016)
[iii] Amin, N., and Douglas, J., Diabetic foot disease: From the evaluation of the “foot at risk” to the novel diabetic ulcer treatment modalities. World J Diabetes, 2016. 7(7): p 153-164. http://www.wjgnet.com/1948-9358/full/v7/i7/153.htm (accessed 7/30/2016)

Who is Dr. Kai O Kaye?
Dr. Kaye is a Board Certified Plastic Surgeon, ISAPS expert, and founder of Ocean Clinic. He specializes in multimodal facial rejuvenation, autologous fat grafting in composite breast augmentation, and total core 360-degree lipo-abdominoplasty (tummy tuck). He developed the PAVE-Facelift, a Peeling-Assisted Volume Enhancing Facelift Technique, and published several new techniques for surgical facial Rejuvenation in peer-reviewed journals.
Where is Ocean Clinic Group
The best plastic and cosmetic surgery clinic specialized in fat transfer. Located in Marbella, Madrid, and Zurich. With more than 15 years of experience and performing more than 1000 surgeries a year. Medical professionals, modern facilities, trust, experience, and security. Come and meet us!
And last but not least, now you can book an appointment online via this
Feel free to contact Dr. Kai O Kaye or Ocean Clinic, experts about your concerns and questions. Remember you can even upload videos or photos describing your problem so that you can get the best response on time.
Contact Information
Email Address: info@oceanclinic.net
Official Website: www.oceanclinic.net
Facebook:www.facebook.com/Oceanclinic
Instagram: www.instagram.com/ocean_clinic/
Related posts:
 What are TOP 5 rejuvenate skin treatments?
What are TOP 5 rejuvenate skin treatments?
 Annika Urm Vitamin IV Therapy experience at Vit&Drip Center Marbella: beyond my expectation
Annika Urm Vitamin IV Therapy experience at Vit&Drip Center Marbella: beyond my expectation
 Come to Training & Boxing with Dilly on the Beach Marbella, San Pedro, Spain 2024
Come to Training & Boxing with Dilly on the Beach Marbella, San Pedro, Spain 2024
 Dr Casabona explains the “HEAT” concept in aesthetic medicine treatments and anti-ageing cosmetics
Dr Casabona explains the “HEAT” concept in aesthetic medicine treatments and anti-ageing cosmetics